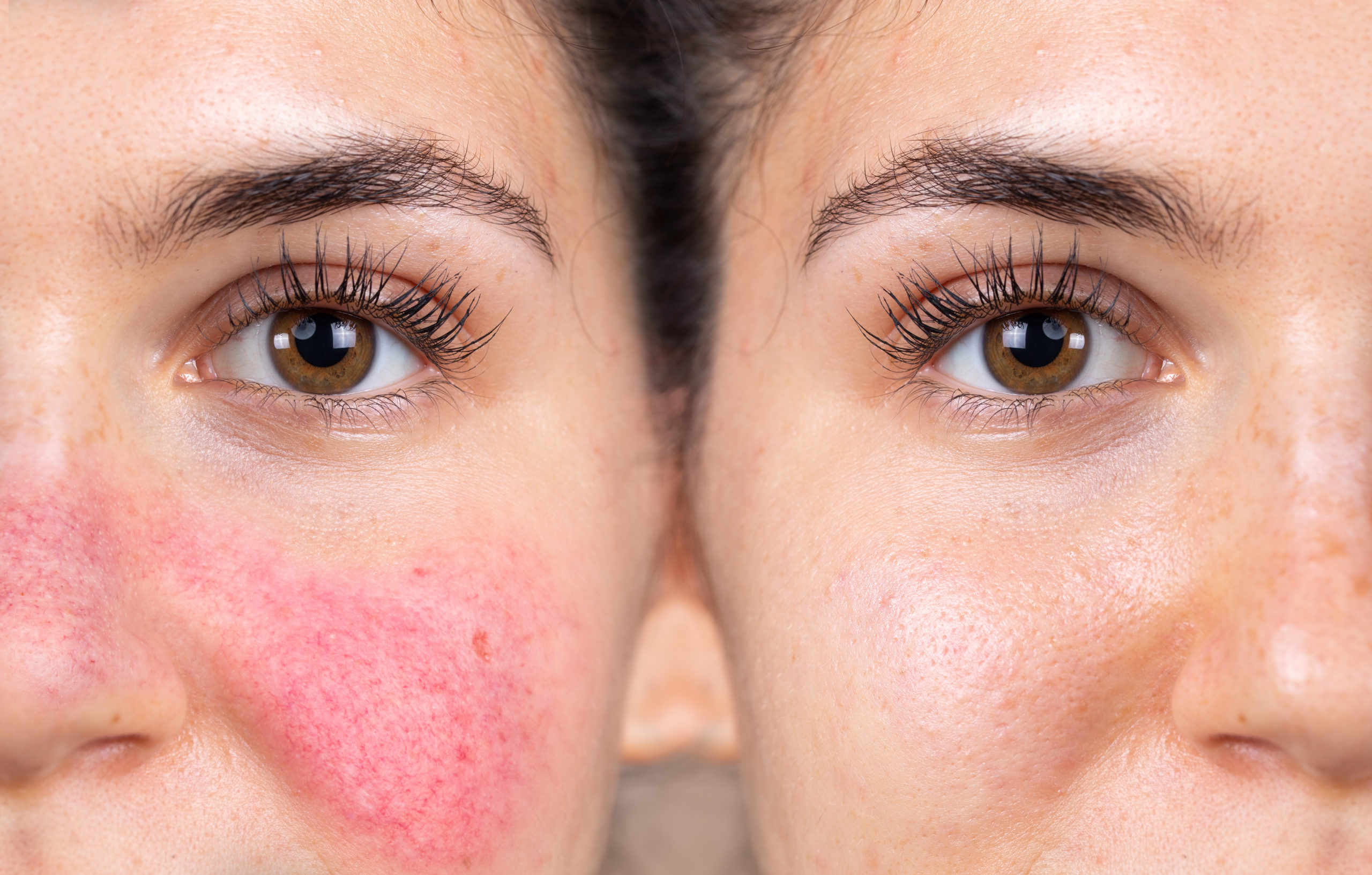
Over the past few decades the number of children that suffer from allergic diseases in western developing countries has increased dramatically. In fact, just between 1950-1995 the prevalence for allergic disease in children increased by 35%.1 In 1989 Dr. Davis Strachan came up with what is now known as the hygiene hypothesis, which suggested the increased allergic disease prevalence was consequently due to decreased contact with infectious microbes during early childhood. He explained how the bacteria that causes infections tend to strengthen the immune system by increasing the microbial diversity of the intestinal flora and triggering the production of regulatory T cells; these cells regulate the production of immunoglobin E (IgE) antibodies that release chemicals that cause allergic reactions.1,2 Atopic dermatitis is an IgE-associated allergic disease, common in children, that has previously been linked to population variations of commensal lactic acid-producing bacteria.1,2 Studies have shown that when Lactobacillus rhamnosus GG (LGG) was given as a probiotic to mothers from 36 weeks pregnant to when they stopped breast feeding, and then directly to the infant for 6-24 months, the risk of developing atopic dermatitis was decreased by about half.1,2 Evidence from these studies suggests that enhancing the intestinal microbiome by introducing specific probiotics at an early stage, can help prevent the onset of atopic dermatitis in high-risk children. The success of these studies has also produced viable evidence to support further investigation into finding different strains of probiotics that could possibly aid in the prevention of other atopic IgE-associated allergic diseases in the future.
References
1.Biosci Microflora. 2011;30(4):119-28. doi: 10.12938/bifidus.30.119. Epub 2011 Nov 17
4.J Allergy Clin Immunol. 2008 Oct;122(4):788-794. doi: 10.1016/j.jaci.2008.07.011. Epub 2008 Aug 31
The microbiome of the gastrointestinal tract has been at the forefront of skin care research, but in the last few years the actual skin microbiome has become a focal point for research on inflammatory dermatological conditions like atopic dermatitis (AD).1,2 The human skin is home to about over million bacteria, fungi and virus per centimeter where species vary depending on a variety of factors including: location on the body, environment, sex, age, diet, and hygiene.1More and more people are becoming susceptible to dermatological conditions due to new lifestyle changes that can potentially alter the microbiome into a state of dysbiosis. Research has shown that introducing certain probiotics topically can treat different conditions by counteracting the imbalance of the microbiome, enhancing skin barrier functions, preventing biofilm formation, and encouraging the growth of beneficial bacteria on the skin.1,3 However, research has also shown that different strains of bacteria have different effects on the microbiome. For instance, Staphylococcus epidermidis promotes skin immune functions while Staphylococcus aureus does the opposite causing an imbalance in the microbiome and making the skin susceptible to pathogenesis.1,3 Understanding the different effects that certain microbiota have on the microbiome of the skin could lead to huge advancements in the skin care world. With every study, scientists get one step closer to cracking the code of how to hack the microbiome of the skin and personalize treatment options for a variety of skin conditions. Nevertheless, one biggest obstacles that they will have to consider is how diverse these microbiomes are from one person to the next.2
References
1. Cates T (2019) Enhancing the Skin Microbiome to Address Inflammatory Dermatologic Conditions. Townsend Letter:50-51.
2.Euromonitor International. 2019. The role of microbiome in the evolution of skincare [PowerPoint slides].
3.JCI Insight. 2018 May 3;3(9). pii: 120608. doi: 10.1172/jci.insight.120608..
Most people take oral probiotics to promote the health of their intestinal microbiome, but it’s now evident that topical probiotics can also benefit the microbiome of the biggest organ of all; the skin. In the past there have been studies that explain how taking oral probiotic supplements could benefit your skin from the inside out, but researchers are beginning to take a new perspective when it comes to probiotics from the outside in. The have begun investigating the possibilities of topically transplanting probiotics directly into the skin microbiome to treat different skin diseases. A study from Myles et.al., 2018 explained how large populations of Staphylococcus aureus (S.aureus) were found in areas affected by atopic dermatitis, and potentially worsening the symptoms. In hopes that they could combat the symptoms with a probiotic for the skin, they decided to try transplanting an “anti-S.aureus” bacteria, Roseomonas mucosa (R.mucosa), to a patient suffering from AD. They found that it was only when R. mucosa was transferred from a healthy volunteer to the affected area of an AD patient, that S.aureus populations decreased along with pruritis, inflammation, redness, and over all intensity of AD symptoms.2 The results of this study highlight how as researchers uncover how different probiotics affect the microbiome of the skin, they can figure out ways to utilize them in creating different treatments for a variety of skin disorders.
References
1.Cates T (2019) Enhancing the Skin Microbiome to Address Inflammatory Dermatologic Conditions. Townsend Letter:50-51.
2.JCI Insight. 2018 May 3;3(9). pii: 120608. doi: 10.1172/jci.insight.120608.